The Doula Model of Care Guiding Principles & Best Practices for Doulas
Copyright 2024 BY PATTY BRENNAN, ALL RIGHTS RESERVED
Excerpted from The Doula Business Guide, 4th Edition
What is the "Doula Model of Care"?
Doulas are coming into the cultural mainstream, and they are not just for birthing and postpartum mothers and their families. The emerging role of the end-of-life doula is gaining traction and helping transform how we approach end-of-life care in the United States and beyond. As training and certification programs for doulas of all kinds expand exponentially, there is a danger that each new player in the field will attempt to assert their brand by re-inventing and re-defining the role of the doula, potentially undermining evidence-based core principles of what it means to be a doula. Since current evidence for birth doulas is well established1 and based on a model of care that is gaining widespread recognition and acceptance by both consumers and medical care providers, it behooves the doula profession to unite in our understanding of the doula model of care, especially as it evolves to serve diverse needs of families throughout the lifespan.
Preliminary definitions are in order as a basis for understanding. A "model of care" broadly defines the way services are delivered. It outlines best practices for a person, population group, or patient cohort as they progress through the stages of a condition or event. It aims to ensure people get the right care, at the right time, by the right team, and in the right place. According to the Agency for Clinical Innovation, models of care have the following key elements:
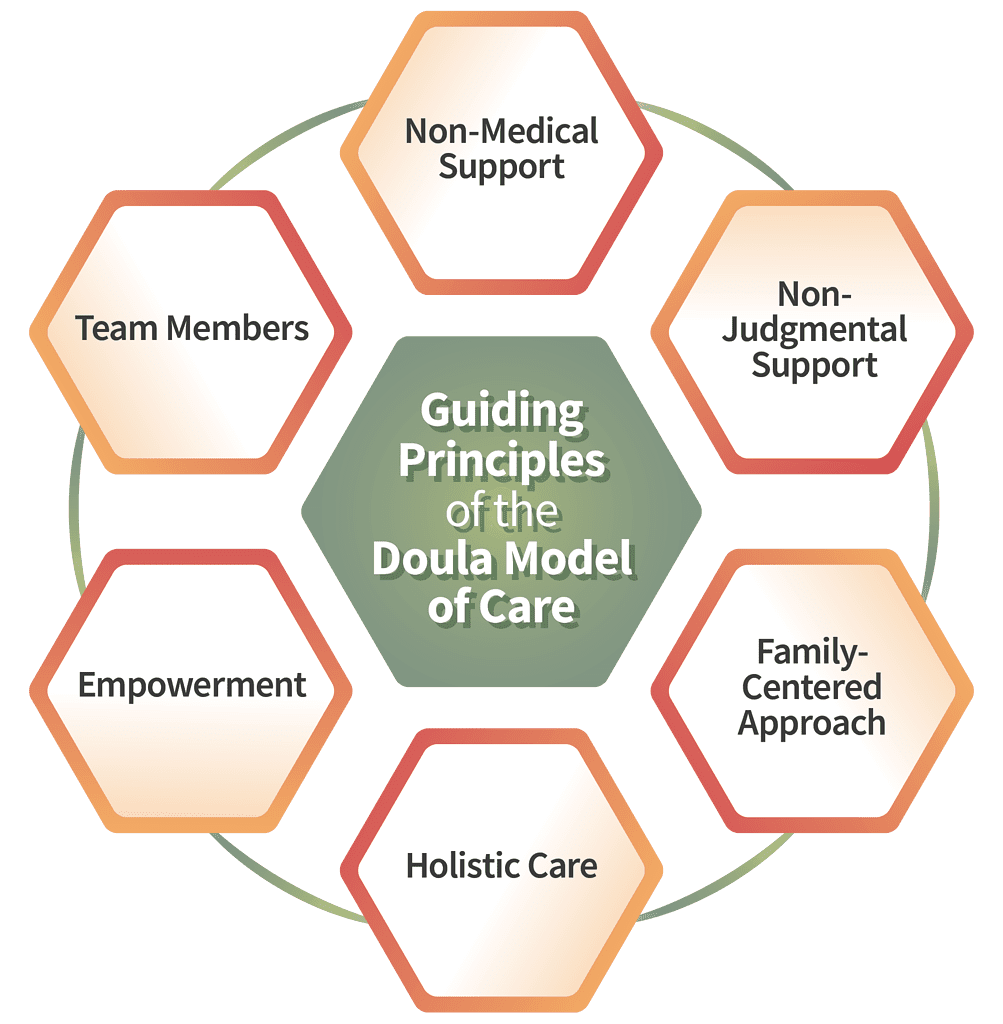
A brief history of doulas
The word Doula has Greek origins and means “one who serves.” Service is at the heart of doula work. Throughout time and in cultures all over the world, there have always been those individuals—usually women—who tend to the needs of the mother in labor, nurture the family in the early weeks postpartum, and care for the sick and dying. The concept of the modern-day doula began in 1969, but the word did not come into widespread use until the early 1990s when professional doula training and certification emerged. A scope of practice for doulas was defined as the time-honored, informal role of the doula became professionalized. Today, there are numerous organizations training and certifying doulas across the globe.
The emergence of the end-of-life doula is a 21st century development, and more men are being drawn into the field. With the “silver tsunami” of aging baby boomers upon us—many of whom are proponents of natural lifestyles and holistic approaches to health care—it makes sense that we are seeking new models of care to meet unmet needs at the end of life.
Each doula business is unique.
Because doulas remain, for the most part, an unregulated profession, there is a great deal of autonomy for doulas to practice freely and evolve businesses that suit each individual doula’s interests, strengths, and skill set. Today, doulas are working in solo practices, partnerships, collectives, and doula agencies. A variety of doula programs have been established, in both the birth and end-of-life arenas, from community-based nonprofits to hospital-based or hospice-sponsored programs. Some doula programs use volunteer doulas only, while others engage doulas as employees or independent contractors.
How each doula manifests the doula model of care and delivers services to families will be uniquely her or his own. There is plenty of room for creative visionaries to adapt the doula model of care for a target demographic or specialized care setting. This freedom, entrepreneurship, and diversity benefit the variety of individuals and families with needs that are unmet by existing systems of care delivery. At the same time, while embracing our diversity, we must acknowledge what unites us as doulas and define the core, non-negotiable elements of the doula model of care.
Support provided by doulas:
Adapting the doula model of care for end of life
If we reconsider the definition and key elements of a “model of care” discussed earlier, the doula model of care readily meets the standards of being high quality, patient centric, collaborative, cost-effective, adaptable, innovative, and visionary.
While the body of literature establishing the benefits of birth doulas is extensive and compelling, standardized outcome measures to evaluate the efficacy of postpartum doulas and, especially, end-of-life doulas are scarce to non-existent. These are urgently-needed areas for research. If the health benefits and cost savings, now in evidence for birth doulas, extends to doulas involved during other critical phases of the lifespan—as we expect they do—then a strong case can be made for expanding third party reimbursement for doulas so more families will benefit.
The more unified the doula profession can be in agreeing on scope of practice, core competencies, and guiding principles for doulas, the more successful we will become. In 2018, the National End-of-Life Doula Alliance (NEDA) was formed by a diverse group of trainers and leaders in the field for this very purpose.4
In terms of linking to national strategic plans and initiatives, the doula model of care synchronizes well with the public health approach to forming “compassionate communities”5 for folks at the end of life now being developed and implemented in Australia, the U.K, Canada, and the U.S. And it is not a hard case to make that the following recommendations of the Institute of Medicine’s landmark report Dying in America (2015)6 are in alignment with the doula model of care:
- Deliver comprehensive end-of-life care by trained caregivers
- Meet Advance Care Planning standards
- Stronger knowledge and skills in palliative care
- Policies and payment systems to support high-quality care
- Public education and engagement
SUMMARY
The emerging field of the end-of-life doula has benefitted from the foundational work completed by leaders in the birth and postpartum doula arena. It would behoove practicing doulas, doula trainers, and hospice and palliative care organizations interested in adopting this new addition to end-of-life care to thoroughly understand and integrate the best of what the established doula model of care has to offer. Within the parameters described, doulas will retain great range for individual expression of their role and the services offered to families. The core principles can serve as a touchstone for the doula profession, helping us to better serve individuals and families while achieving greater recognition and acceptance worldwide.
1Knocke, K., Chappel, A., Sugar, S., De Lew, N., and Sommers, B. (2022). Doula Care and Maternal Health: An Evidence Review. Retrieved from https://aspe.hhs.gov/sites/default/files/documents/dfcd768f1caf6fabf3d281f762e8d068/ASPE-Doula-Issue-Brief-12-13-22.pdf.
2Agency for Clinical Innovation (2013). Understanding the process to develop a model of care: An ACI framework. Retrieved from https://aci.health.nsw.gov.au/__data/assets/pdf_file/0009/181935/HS13-034_Framework-DevelopMoC_D7.pdf.
3DONA International (2020). Birth and Postpartum Doula Standards of Practice and Code of Ethics. Retrieved from https://www.dona.org/what-is-a-doula/scope-and-ethics/.
4National End-of-Life Doula Alliance (NEDA) (2018). Our Scope of Practice. Retrieved from https://www.nedalliance.org/scope-of-practice.html.
5Librada-Flores, S., Nabal-Vicuña, M. Forero-Vega, D., Muñoz-Mayorga, I., and Guerra-Martin, M. (2020). Implementation models of compassionate communities and compassionate cities at the end of life: A systematic review. Int J Environ Res Public Health. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7504622/.
6Institute of Medicine (2015). Dying in America. Improving quality and honoring individual preferences near the end of life. Retrieved from https://nap.nationalacademies.org/catalog/18748/dying-in-america-improving-quality-and-honoring-individual-preferences-near.
